The Commonwealth Fund, a well-respected think tank focused on promoting a high-performance and equitable healthcare system, published a primer on the 340B program last week, highlighting the program’s growth and the controversy its growth has sparked.
“We did the report because 340B is often in the news and there are many developments with it, so we wanted to provide some context and information on it for our audience,” Lovisa Gustafsson, the group’s vice president, controlling healthcare costs, told 340B Report. “We do realize it is a very complex topic and not all aspects of the program were addressed in the piece we put out.” She said the Commonwealth Fund may follow up with additional pieces on the 340B program “if this continues to be an area of interest.”
The Sept. 8 article noted that the 340B program’s rapid growth since its 1992 inception has pitted drug manufacturers against 340B providers and federal policymakers and has spawned a series of ongoing legal battles.
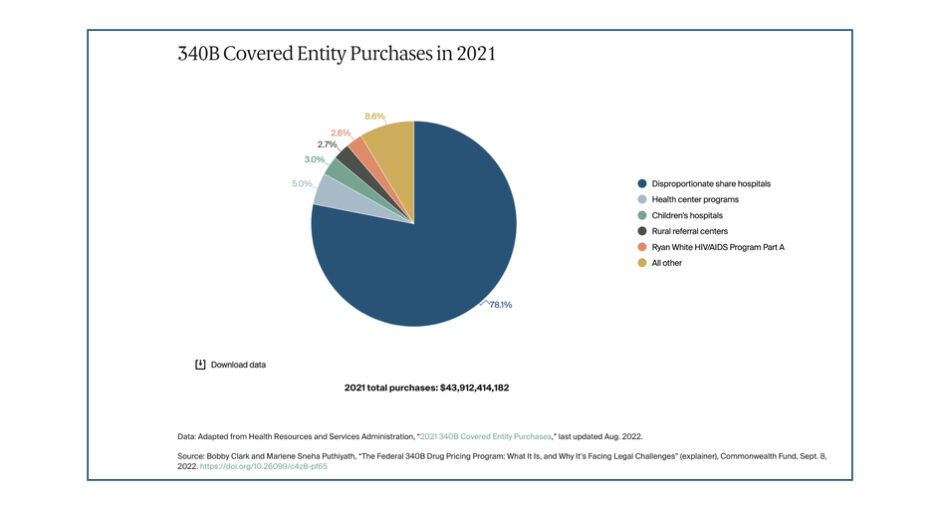
“Drug manufacturers are alarmed about the program’s fast expansion,” it said, noting that 340B provider sites, including both hospital and pharmacies, grew to 50,000 sites by 2020 from 8,100 sites in 2000. Meanwhile, drug purchases under the program reached $44 billion last year, about 16% more than in 2020, the article noted.
The article said the 340B program’s rapid expansion is attributable largely to the 2010 passage of the Affordable Care Act, which increased the number and type of entities eligible under the program, and to a 2010 policy change that allowed 340B providers to use an unlimited number of contract pharmacies.
The article lays out the arguments on both sides of the contract pharmacy dispute, with drug makers claiming the 340B statute does not expressly allow the use of contract pharmacies, that the program lacks transparency and oversight, and that 340B savings are not being passed on to patients but instead are boosting providers’ profits.
It noted drug makers’ move to impose conditions on 340B entities’ use of contract pharmacies, such as requiring the submission of claims level data, a policy that has given rise to a number of legal disputes.
The article said 340B providers counter that policymakers intentionally expanded the 340B program to address the fact that a significant amount of the care provided to millions of uninsured patients goes uncompensated, and that, in any case, 340B drug discounts represent a small percentage of total U.S. sales, with 340B drug purchases comprising about 7 percent of total drug sales in 2020.
“With cases still ongoing, the legal and regulatory landscape is still very much in flux,” the article said. “It remains to be seen how these disputes will be resolved and what kind of impact they will ultimately have on the size and scope of the 340B drug discount program.”
As for policymakers’ response, the article noted, “For the moment, it appears that most policymakers side with 340B entities and believe that the drug discount program is an important tool for safety-net providers.”
For example, the Biden administration has weighed in, saying the restrictions drug manufacturers are imposing on 340B providers are violating the law, resulting in 340B entities paying more than the discounted price they are eligible to receive, it said.
Also, a bipartisan group of six lawmakers led by Rep. Abigail Spanberger (D–Va.) recently wrote a letter to the U.S. Department of Health and Human Services urging the agency to take action against drug makers that are violating the 340B law, the article noted.
The six lawmakers followed up in July with a similar bipartisan letter signed by 181 House members. U.S. Health and Human Services Secretary Xavier Becerra responded on Sept. 1. He said HHS is doing all it can with the tools it has to address drug manufacturers’ denials of 340B pricing involving contract pharmacies. If lawmakers want his department to do more, they should give it more regulatory power over 340B and more money for audits and oversight, he said.